Symptoms of psoriasis
The main symptom of psoriasis is dry, itchy, sore, flaky patches of skin that form what look like silvery-white scales.
Psoriasis patches are usually:
- 1 to 2cm in size
- an oval or irregular shape.
- pink or red on white skin, turning silvery-white, and can sometimes turn a waxy yellow or orange-brown colour
- grey on brown or black skin, and cause dark marks on the skin after the psoriasis has gone
Most people only get a few psoriasis patches, but others get them across large parts of their body. Some people have lots of smaller, scaly patches.
You may also get lots of small brown and yellow spots on the palms of your hands and soles of your feet.
You can get psoriasis in different parts of your body, but it's mostly found on the:
- head and behind the ears
- chest, tummy and back
- bottom
- forearms and elbows
- lower legs and knees
You can also get it in the folds of your body, such as your groin, genitals and under your breasts, or on your fingernails. The surface of your nails can have dents and pits.
You can get psoriasis at any age, but symptoms often start either between the ages of 15 and 25, or 50 and 60 .
There are usually times where your symptoms get worse (called flare-ups) and times when they're better.
- 1: White skin with patches of psoriasis on the arm (thumbnail).
- 2: Dark brown skin with patches of psoriasis on the forearm (thumbnail).
- 3: The fingernail of a person with psoriasis (thumbnail).
Long description, image 1.
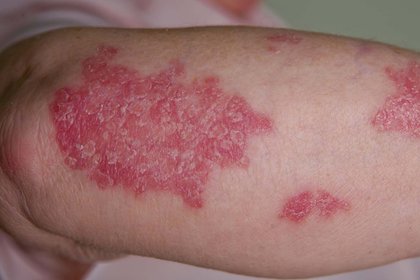
Psoriasis patches on the arm of someone with white skin.
Areas of the skin are pink and red with lighter scales. Some of the patches are larger and others are smaller.
Long description, image 2.
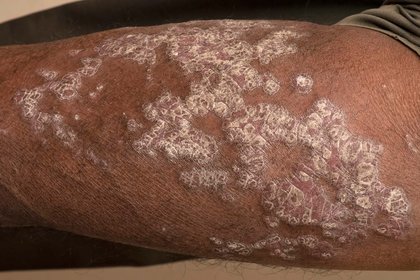
Psoriasis on the forearm of someone with dark brown skin.
Areas of the skin look grey, white, raised and scaly. The patches have joined together in places to form a larger patch.
Long description, image 3.
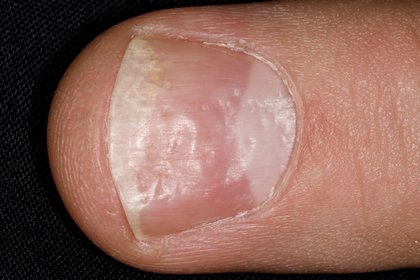
The fingernail of a person with nail psoriasis.
The nail has several small pits and dents, as well as thicker, whiter areas near the tip.
Some people with psoriasis can develop psoriatic arthritis as they get older. This is an inflammatory condition that affects the joints.
Non-urgent advice: See a GP if:
- you have symptoms of psoriasis
- you have psoriasis and your treatment is not working or is giving you side effects
- you have psoriasis and also have pain, stiffness and swelling in your joints that keeps coming back
Immediate action required: Call 999 or go to A&E if:
You have psoriasis and:
- your skin quickly turns red and you develop white, pus-filled bumps that join together – redness may be harder to see on brown or black skin
- have psoriasis patches on your feet that turn yellow-brown and are filled with pus
- your fingers and toes have red, scaly pus-filled bumps on the tips – redness may be harder to see on brown or black skin
These can be signs that you have a more serious condition or an infection.
You may also have other symptoms such as your heart beating fast, or a high temperature, or feeling hot, cold or shivery.
Find your nearest A&EDo not drive to A&E. Ask someone to drive you or call 999 and ask for an ambulance.
Bring any medicines you take with you.
Treatment for psoriasis
How your psoriasis is treated depends on the type of psoriasis you have, how severe it is, and where it is on your body.
The main treatments are:
- vitamin D creams, lotions, ointments and gels
- moisturising creams, lotions, ointments and gels for your skin and to wash with (emollients)
- steroid creams, lotions or gels
- other treatments for your skin or scalp, such as coal tar
If your psoriasis is more severe, there are other treatments, such as light therapy and medicines.
You may need a combination of different treatments.
A GP can prescribe some treatments, or you may be referred to a skin specialist (dermatologist).
Living with psoriasis can be difficult. If it affects your mental health, you may be referred to a mental health specialist.
Causes of psoriasis
Psoriasis is caused by your skin making more skin cells than usual, which creates patches on the skin.
It's not known why or how this happens, but it's thought to be caused by a problem with the immune system.
You're more likely to have it if a member of your family has psoriasis.
There are certain things that can make your psoriasis worse or cause a flare-up of symptoms (triggers).
Triggers can include:
- stress
- drinking alcohol or smoking
- living with obesity
- being pregnant
- certain medicines
- infections, such as strep A and HIV
- cuts, scratches or grazes on your skin
- sunlight
Psoriasis is not contagious so you cannot catch it or spread it.
Things you can do to help with psoriasis
There are things you try that can help with psoriasis.
Do
-
try to avoid the things that make your symptoms worse (triggers)
-
have a healthy, balanced diet
-
get regular exercise
-
try to reduce stress if you can
-
try not to drink too much alcohol
-
try to stop smoking, if you smoke
Don’t
-
do not share your moisturising treatments (emollients) with anyone else
-
do not put your fingers into a pot of emollient – use a spoon, spatula or pump dispenser instead
-
do not smoke or go near naked flames if you use an emollient – clothing and bedding that's been in contact with an emollient burns more easily
More information
NHS Better Health has free tools and support to help you get active, quit smoking and drink less
Complications of psoriasis
If you have psoriasis, there's a higher chance that you may develop other health issues.
You'll have regular check-ups and get advice on how to manage your health to reduce your chance of developing these conditions.
Complications of psoriasis can include:
- psoriatic arthritis
- metabolic syndrome, which can lead to conditions such as diabetes, cardiovascular disease and DVT (deep vein thrombosis)
- inflammatory bowel disease, such as Crohn's disease
Speak to your doctor if you notice any new symptoms or have any concerns.
Psoriasis in pregnancy
You may need to change your treatment if you have psoriasis and you're planning to have a baby or are pregnant, as some medicines can be harmful.
Pregnancy can sometimes also make your symptoms worse.
Speak to your doctor or a pharmacist if you're pregnant or trying to get pregnant.
Help and support for psoriasis
Psoriasis can be a difficult condition to live with and it's common for it to affect your mental health.
As well as support from your GP, you may find it helpful to get support from other people with psoriasis, either at a local support group or online.
There are also national charities that offer support and information about psoriasis.
Psoriasis Association
Information and support for anyone affected by psoriasis.
- Website: www.psoriasis-association.org.uk
PAPAA (Psoriasis and Psoriatic Arthritis Alliance)
Information and support for anyone affected by psoriasis.
- Website: www.papaa.org
- PAPAA: community forum
Page last reviewed: 10 March 2026
Next review due: 10 March 2029