Why the 20-week scan is done
The 20-week scan is done to check if your baby could have a condition that affects their health and development.
Your baby will be checked for signs of 11 different conditions as part of the scan.
Some conditions can be seen more clearly than others, so the scan may not find everything. But screening is the best way to find any conditions, and help you and your doctors make the best decisions for you and your baby.
Your placenta and the blood flow in your uterus will also be checked.
Show the 11 conditions the scan checks for
During the 20-week scan your baby will be checked for signs of:
- anencephaly
- open spina bifida
- cleft lip and palate
- diaphragmatic hernia
- gastroschisis
- exomphalos
- serious cardiac abnormalities
- bilateral renal agenesis
- severe skeletal dysplasia
- Edwards' syndrome (trisomy 18)
- Patau's syndrome (trisomy 13)
Who the 20-week scan is for
A 20-week scan is always offered when you're pregnant. It's usually done when you're between 18 and 21 weeks pregnant.
How to get the 20-week scan
Your midwife will tell you how to book the 20-week scan. How you book depends on which area of the country you are in.
You may:
- be given a form to fill in after your first midwife appointment
- need to book the appointment after your 12-week scan
- need to call your local hospital to book the scan
- get a letter in the post with a prebooked appointment
- need to book the appointment using an app
You'll usually have the scan before you're 21 weeks pregnant, but you're able to have it up until you're 23 weeks pregnant in some cases.
You'll also be told if you need to have a full bladder before the scan.
If you've not had a 20-week scan and you're between 18 and 23 weeks pregnant, tell your midwife or GP.
It's your choice if you want to have a 20-week scan or not. The scan is the best way to find out if your baby has one of the 11 conditions, but not everyone wants this information. Talk to your midwife about your options.
If you decide not to have it but change your mind later, speak to your midwife or GP. They can tell you if you're still able to have the scan.
Preparing for the 20-week scan
There are things you can do to prepare for your 20-week scan.
Do
-
arrive for your appointment early
-
wear loose clothing that's easy to move to get to your tummy
-
take out a belly piercing, if you have one
-
bring your maternity notes with you, if you have paper notes
-
make sure you have a full bladder before the scan, if you've been told to
-
check with the hospital or clinic before your appointment if you'll need to pay for pictures of your baby
Important
You can bring someone to the scan with you, but most hospitals do not allow children. Check with the clinic or hospital before your appointment.
How the 20-week scan is done
Your 20-week scan is usually done at a local hospital, clinic or health centre by a trained healthcare professional.
The ultrasound scan usually takes around 30 minutes. There's no known risk to you, or your baby, from the scan.
The scan can sometimes take longer if your baby is moving around a lot or is not in the right position to get clear pictures.
If this happens, you may be asked to go for a walk or eat something before coming back after a short break so all the checks can be done.
If it's still difficult to get clear pictures of your baby, you'll be offered another appointment before you're 23 weeks pregnant.
The scan cannot find all conditions. If you have any symptoms you're worried about or something does not feel right, it's important to tell your midwife.
During the scan
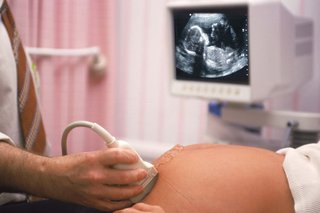
- The ultrasound scan will take place in a dimly lit room to get clear pictures of your baby.
- You'll be asked to lie on a couch and to lift or lower your clothing so the healthcare professional can see and touch your tummy.
- Tissue paper will be tucked into your clothing before a cold gel is put on your tummy.
- The healthcare professional will move a handheld device called a probe over your tummy so they can see a picture of your baby and check their body. This may be uncomfortable.
- They may be quiet while they look closely at your baby's bones, heart, brain, spinal cord, face, kidneys and tummy. They'll also check your placenta and the blood flow in your uterus.
- Sometimes the healthcare professional may ask another member of the team to check the picture of your baby.
- You may be asked if you'd like to know the sex of your baby.
Getting the results of your 20-week scan
You'll be told the results of the 20-week scan after the healthcare professional has done all the checks.
Most people will be told their baby does not have any signs of a condition.
But some people may be told their baby has signs of one of the conditions being checked for.
If your baby has signs of a condition
You'll be told if there are signs your baby may have a health condition after the scan.
If the ultrasound scan finds something, you may be offered more scans and tests, such as amniocentesis or chorionic villus sampling.
You'll be referred to a specialist, who will tell you more about the tests to help you decide if you want to have them.
These tests will be able to tell you if your baby definitely has a health condition and what this means for you and your baby.
Find out more about what happens if antenatal screening tests find something and about having a baby that might be born with a condition.
Get support
Antenatal Results and Choices (ARC) has information about screening tests and how you might feel if you're told your baby has, or might have, a condition.
Their helpline is open Monday to Friday, 10am to 5.30pm.
Call 020 7713 7486.