Symptoms of slapped cheek syndrome
The first sign of slapped cheek syndrome is usually feeling unwell for a few days.
Symptoms may include:
- a high temperature
- a runny nose and sore throat
- a headache
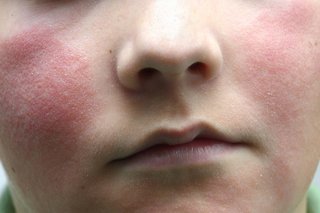
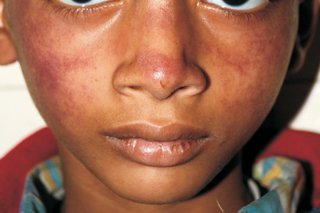
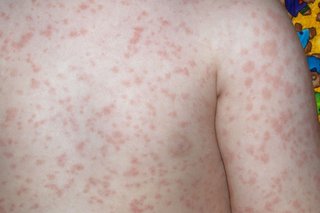
How long it lasts
The rash usually fades within 1 to 3 weeks, but it can sometimes last for longer, especially if you're hot or stressed.
Adults might also have joint pain and stiffness. This can happen in children too, but it's rare. Joint pain can continue for many weeks, even after the other symptoms have gone.
If you're not sure your child has slapped cheek syndrome
Look at other rashes in babies and children.
How to treat slapped cheek syndrome yourself
You do not usually need to see a GP for slapped cheek syndrome.
There are some things you can do to ease the symptoms.
Do
-
rest
-
drink plenty of fluids to avoid dehydration – babies should continue their normal feeds
-
take paracetamol or ibuprofen if uncomfortable
Don’t
-
do not give aspirin to children under 16
Important
Tell your midwife or a GP if you're pregnant or have a weakened immune system or blood disorder and have been near someone with slapped cheek syndrome.
Non-urgent advice: See a GP if:
You think you have slapped cheek syndrome and:
- you're pregnant – there's a very small risk of miscarriage or other complications
- you have a blood disorder, such as sickle cell disease or thalassaemia – there's a risk of severe anaemia
- you have a weakened immune system – for example, because of chemotherapy, leukaemia, HIV or diabetes
Urgent advice: Ask for an urgent GP appointment or get help from NHS 111 if:
You think you have slapped cheek syndrome and you have:
- very pale skin
- shortness of breath
- extreme tiredness
- fainted
These can be signs of severe anaemia and you might be sent to hospital for a blood transfusion.
You can call 111 or get help from 111 online.
How slapped cheek syndrome is spread
Slapped cheek syndrome is caused by a virus (parvovirus B19). The virus spreads by coughs and sneezes or by touching contaminated objects.
It's hard to avoid spreading slapped cheek syndrome because most people do not know they have it until they get the rash.
You can only spread it to other people before the rash appears.
To reduce the risk of spreading the virus:
- wash your hands often with water and soap
- use tissues to trap germs when you cough or sneeze
- bin used tissues as quickly as possible
You do not have to stay off work or school after the rash appears.
Let the school or teacher know if your child has slapped cheek syndrome.
Page last reviewed: 18 April 2024
Next review due: 18 April 2027
Image provided by Indian Pediatrics: Slapped cheek syndrome (Indian Pediatrics; PDF only, 36KB)