Why lumbar decompression surgery is done
You may need lumbar decompression surgery if:
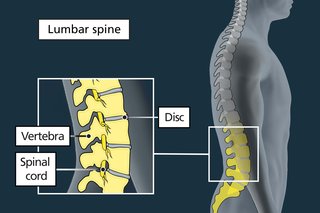
- the space inside each bone in your spine (vertebra) has become too narrow because of changes that can happen with age or arthritis (spinal stenosis)
- the nerve that sends messages between your spine and legs (sciatic nerve) is compressed (sciatica)
- one of the small cushioning discs between the bones in your spine has moved out of place (slipped disc)
- the nerves at the base of your spine are compressed (cauda equina syndrome)
- you've had a spinal injury, such as fractured vertebra
- you have a tumour or build-up of pus (abscess) in your spine
Depending on the cause of your compressed nerves, you may have other treatments first, such as physiotherapy, losing weight if you're overweight, or steroid injections.
What happens during lumbar decompression surgery
Lumbar decompression surgery is done in hospital.
It can be done several ways, depending on the condition you have. Your surgeon should talk to you about how they plan to do the operation.
The hospital will give you information about how to prepare for the operation, such as when you can eat or drink and any medicines you should stop taking before surgery.
You'll be given a general anaesthetic before the operation, so you'll be asleep and will not feel any pain.
During the operation:
- Your surgeon will make 1 large cut in your skin, usually in your back, or several small cuts.
- They'll removes small pieces of bone from a vertebra (called a laminectomy). Sometimes a part of the cushion between each vertebra (a disc) is also removed (called a discectomy).
- The wound may be closed with dissolvable stitches, or clips and stitches that will be removed after the wound has healed.
The operation usually takes around 2 to 4 hours, but may take longer.
After the operation
You'll wake up in a recovery area and have medicine to help with pain and swelling before you're taken to a ward.
You'll usually have a drip in a vein in your arm giving you fluid and medicine. You may also have a tube called a catheter in your bladder, to drain your pee into a bag. This is usually removed after 1 or 2 days.
Your nursing team will help you to get up and move around as soon as possible after surgery. Depending on how your operation was done, and the reason you had it, you may be able to leave hospital after around 2 to 5 days.
Recovery after lumbar decompression surgery
You may be able to return to work around 4 to 6 weeks after your operation, depending on the type of work you do and the advice from your doctor.
It may take up to 12 weeks for you to be able to do all your usual activities.
You may need to take painkillers for several weeks after surgery. The hospital should also give you information about how to look after your wounds at home and any activities you may have to avoid while you recover, such as driving or contact sports.
It's important to follow the advice you get from your healthcare team so you have a good recovery.
The hospital might also arrange for you to have:
- physiotherapy to help with your movement after surgery
- occupational therapy to help make everyday tasks easier while you recover
Possible complications of lumbar decompression surgery
Your doctor will talk to you about the possible complications of having lumbar decompression surgery.
Serious complications are uncommon but may include:
- a leak of spinal fluid, which may mean more surgery is needed
- damage to spinal nerves or paralysis, where you lose feeling and movement from below your waist
- back pain that does not get better
- other bones in your spine (vertebrae) moving out of place after surgery, which may mean another operation is needed
Urgent advice: Contact the hospital or NHS 111 if:
You have had lumbar decompression surgery and:
- get new symptoms, such as pain, weakness or numbness in your legs, or problems controlling when you pee or poo
- the skin around your stitches is hot, itchy, oozing fluid or red (redness may be harder to see on black and brown skin)
You can call 111 or get help from 111 online.
Page last reviewed: 10 March 2026
Next review due: 10 March 2029