What's happening in my body?
If this is your first baby, then you'll have an antenatal appointment this week. Your blood pressure will be checked, your bump will be measured and you'll hand over a urine sample.
Your midwife or doctor will be checking for signs of pre-eclampsia, a dangerous condition that's characterised by high blood pressure and protein in the urine.
You're probably getting a lot of practice contractions now, which should not be painful. These are Braxton Hicks contractions.
When you start getting labour pains, you'll know all about it! Real contractions hurt when your bump goes tight, and then the pain goes away when the muscles relax.
Labour is divided into 3 stages. The first stage is when you have contractions and your cervix opens up until it's 10cm across (fully dilated). The 1st stage lasts 6 to 12 hours, or less if you've had other children.
The 2nd stage is where the baby is delivered – and the 3rd stage is when the placenta comes out.
Find out more about the stages of labour and birth on the NHS website.
When your contractions last for at least 60 seconds and come every 5 minutes, call your hospital or midwife.
RSV vaccination
Have you had the RSV (respiratory syncytial virus) vaccine? It's usually offered at around week 28 but can be given later if needed, right up until you go into labour.
Having the vaccination can lower your baby's risk of a severe lung infection called bronchiolitis, which can make it difficult for your baby to breathe and feed. If you've not had it yet, speak to your midwife or a GP.
From breathing to bananas: 8 tips for your labour
These tips could help you feel in control and manage your pain:
- If your contractions start at night, try to sleep your way through as much as possible. The rest will help to prepare you for the birth, and your cervix will dilate while you sleep.
- If your contractions start in the day, then keep upright and active, as this helps the baby to move down and your cervix to open up. This could speed up your labour and reduce the need for painkilling drugs.
- Try different positions. Rock on a birth ball, or put your arms around your birth partner's neck and lean on them. Just keep moving.
- Have a warm bath or shower – it's a tried and tested method of pain relief.
- Focus on breathing. You can practise your breathing techniques now. Take deep breaths in through your nose and out through your mouth. Keep your jaw relaxed.
- Ask your birth partner for a massage and involve them in your labour. Having their support and reassurance will encourage your body to produce more endorphins, which are brilliant natural painkillers. The NHS website has more suggestions on how your partner could support you.
- Eat something healthy to keep up your energy levels, like a banana or low-fat yoghurt. Avoid fatty foods, as they could make you feel sick, and steer clear of sugary foods, as they'll only give you a quick hit before a slump.
- Do something that helps you to relax. If you feel calm, you will be able to manage your labour and pain much better than if you're stressed.
Will curries and sex bring on labour?
You've probably searched the internet for ways to bring on labour and found tips that range from sex to vindaloos.
Tommy's has information on what might help bring on labour, from raspberry leaf tea to nipple stimulation.
There are no proven ways to safely bring on labour at home. Get advice from your doctor or midwife before trying anything other than watching and waiting.
3rd trimester pregnancy symptoms (at 40 weeks)
Do you feel like you've got PMT? Or do you have lower backache? These could be early signs of labour. Check out these 5 signs that your baby is on the way.
Your signs of pregnancy could also include:
- painless contractions around your bump, known as Braxton Hicks contractions
- sleeping problems (week 19 has information on feeling tired)
- stretch marks (week 17 has information on stretch marks)
- swollen and bleeding gums (week 13 has information on gum health during pregnancy)
- pains on the side of your baby bump, caused by your expanding womb ("round ligament pains")
- piles (week 22 has information on piles)
- headaches (read about headaches in pregnancy on NHS.uk)
- backache
- indigestion and heartburn (week 25 has information on digestive problems)
- bloating and constipation (week 10 has information on bloating)
- leg cramps (week 20 has information on how to deal with cramp)
- feeling hot
- dizziness
- swollen hands and feet
- urine infections
- vaginal infections (week 15 has information on vaginal health)
- darkened skin on your face or brown patches – this is known as chloasma or the "mask of pregnancy"
- greasier, spotty skin
- thicker and shinier hair
You may also experience symptoms from earlier weeks, such as:
- mood swings (week 8 has information on mood swings)
- morning sickness (week 6 has information on dealing with morning sickness)
- weird pregnancy cravings (week 5 has information on pregnancy cravings)
- a heightened sense of smell
- sore or leaky breasts (week 14 has information on breast pain) – a white milky pregnancy discharge from your vagina and light spotting (seek medical advice for any bleeding)
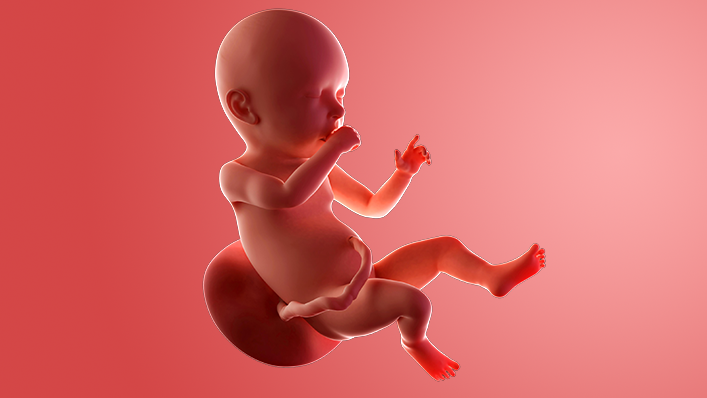
What does my baby look like?
Your baby, or foetus, is around 51.2cm long from head to heel. That's approximately the size of a pumpkin.
Your baby is getting rather squashed up now, but should still be moving around in their usual pattern. Movements should not slow down or stop, and if they do, it could be an important sign that something is wrong.
If you notice any changes, contact your midwife or maternity unit straight away – there will be someone there to answer calls 24 hours a day.

Action stations
Be on full alert in case your waters break, as this could happen at any time. Don't expect a tidal wave, as it could be just a trickle.
If you think it's started, then call your midwife or doctor and ask for advice.
You might have just wet yourself, but if your waters have broken, then your labour may need to be induced, as your baby will be at a greater risk of infection.
This week you could also...

Baby basics
From the essentials of caring for your baby to understanding their sleep, find out all the baby basics you need to know about your newborn.