Chilblains are small, itchy patches that can appear on your skin after you've been in the cold. They usually clear up on their own. You may need to see a GP if they do not go away.
Check if you have chilblains
Chilblains usually appear a few hours after you've been in the cold.
You mostly get them on your fingers and toes. But you can also get them on your face and legs.
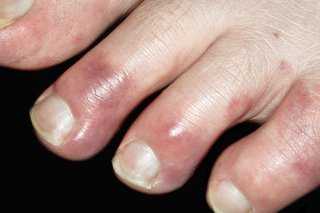
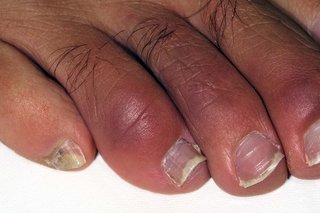
What you can do about chilblains
Chilblains usually go away on their own in 2 to 3 weeks.
There are some things you can try to get rid of them yourself and stop them coming back.
Do
-
try to avoid being outside when it's cold or damp – if you do go out, wear warm, waterproof clothing, gloves and thick socks
-
take paracetamol or ibuprofen to ease the pain
Don’t
-
do not put your feet or hands on a radiator or under hot water to warm them up
-
do not smoke or have drinks that have caffeine in them – this can affect the flow of blood in your fingers and toes
-
do not scratch or pick at your skin
Some painkillers are not safe for everyone (for example, if you're pregnant). Always check the leaflet or get medical advice before taking them.
A pharmacist can help with chilblains
You can ask a pharmacist about:
- the best painkiller to take
- creams that can help to soothe the itching
- if you need to see a GP
Non-urgent advice: See a GP if:
- you have chilblains and your skin has not got any better after 2 to 3 weeks
- there is pus coming out of your skin
- your temperature is very high or you feel hot or shivery
- you keep getting chilblains
- you have diabetes and have chilblains – foot problems can be more serious if you have diabetes
What happens at your appointment
A GP will check your symptoms to see if you have chilblains.
They may need to refer you for further tests with a specialist if they're not sure why you're getting chilblains.
Rarely, the GP will prescribe a medicine that can help your chilblains clear up.
Causes of chilblains
You can get chilblains when it's cold. The cold makes the tiny blood vessels in your fingers and toes get smaller. This stops blood moving around as easily.
If you warm up too quickly, the blood vessels get bigger again and blood rushes to your fingers and toes. This can cause pain or swelling.
Page last reviewed: 29 July 2022
Next review due: 29 July 2025