Shingles is an infection that causes a painful rash. Get advice from 111 as soon as possible if you think you have it.
Check if you have shingles
The first signs of shingles can be:
- a tingling or painful feeling in an area of skin
- a headache or feeling generally unwell
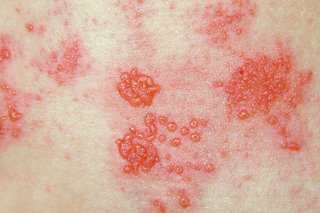
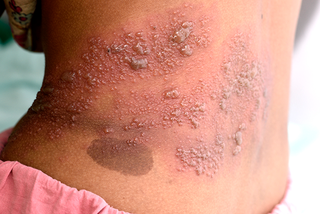
A rash will usually appear a few days later. In rare cases shingles can cause pain without a rash.
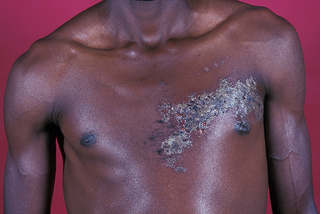
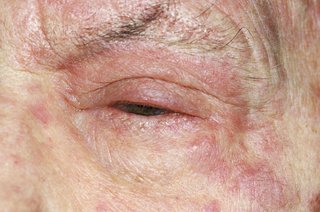
Usually you get the shingles rash on your chest and tummy, but it can appear anywhere on your body including on your face, eyes and genitals.
The rash appears as blotches on your skin, on 1 side of your body only. A rash on both the left and right of your body is unlikely to be shingles.
Urgent advice: Ask for an urgent GP appointment or get help from NHS 111 if:
- you think you might have shingles
You might need medicine to help speed up your recovery and avoid longer-lasting problems.
This works best if you start taking it within 3 days of the shingles rash appearing.
You can call 111 or get help from 111 online.
A pharmacist can help with shingles
You can also speak to a pharmacist if you think you have shingles. They can provide the same treatments you would get from a GP, if you need it.
Treatment for shingles
Treatment for shingles depends on how severe your symptoms are and whether you're at risk of complications.
If you have a mild rash you may not need any treatment.
You may be offered medicine (antiviral tablets) to help speed up your recovery from shingles if:
- you have a weakened immune system
- your pain or your rash is moderate or severe
- the rash is affecting other areas of your body apart from your chest, tummy and back
You usually need to start taking the medicine within 3 days of your rash first appearing.
Treatment for shingles can also include medicines to help relieve pain, such as painkillers, steroid tablets or medicines that help with nerve pain.
Shingles medicines from a pharmacy
If you have shingles, you may be able to get antiviral tablets from some pharmacies without seeing a GP.
How to treat shingles symptoms yourself
If you have shingles there are things you can do to help with the symptoms.
Do
-
take paracetamol to ease pain
-
keep the rash clean and dry to reduce the risk of infection
-
wear loose-fitting clothing
-
use a cool compress (a bag of ice cubes or frozen vegetables wrapped in a towel, or a wet cloth) a few times a day
Don’t
-
do not let dressings or plasters stick to the rash
-
do not wear clothes with rough fibres that can irritate your skin
How long shingles lasts
It can take up to 4 weeks for the shingles rash to heal.
Your skin can be painful for weeks after the rash has gone, but it usually gets better over time.
Stay away from certain groups of people if you have shingles
You cannot spread shingles to others. But people could catch chickenpox from you if they have not had chickenpox before or have not had the chickenpox vaccine.
This is because shingles is caused by the chickenpox virus.
Try to avoid:
- anyone who is pregnant and has not had chickenpox before
- people with a weakened immune system – like someone having chemotherapy
- babies less than 1 month old
Important: Work and school
Stay off work or school if the rash is still oozing fluid (weeping) and cannot be covered, or until the rash has dried out.
You can only spread the infection to other people while the rash oozes fluid.
You can cover the rash with loose clothing or a non-sticky dressing.
Complications of shingles
Most people recover from shingles without any problems. But it can sometimes cause complications, such as:
- post-herpetic neuralgia, where pain lasts for several months after the shingles rash has gone
- the rash becoming infected, which may need to be treated with antibiotics
- scarring or changes in skin colour after the rash has healed
- muscle weakness
- eye problems, which can lead to sight loss
- Ramsay Hunt syndrome, a rare condition where shingles affects your facial nerve, causing weakness on one side of your face and sometimes hearing problems
You can reduce the risk of complications by getting treatment as soon as possible after your symptoms start.
Shingles and pregnancy
If you're pregnant and get shingles, it's mostly mild and there's usually no risk to you or your baby.
But a GP should arrange for a specialist to advise on whether you need treatment.
Causes of shingles
You cannot get shingles from someone with shingles or chickenpox.
But you can get chickenpox from someone with shingles if you have not had chickenpox before.
When people get chickenpox, the virus stays in the body. It can be reactivated later and cause shingles if someone's immune system is weakened.
This can be because of stress, certain conditions, or treatments like chemotherapy.
Shingles vaccine
A shingles vaccine is available on the NHS for:
- people who turned 65 on or after 1 September 2023
- people aged 70 to 79 who have not yet been vaccinated
- people aged 50 and over with a severely weakened immune system
The vaccine helps reduce your risk of getting shingles.
If you get shingles after being vaccinated, the symptoms can be much milder.
You can get shingles more than once, so it's important to get vaccinated even if you've had shingles before.
Ask your GP surgery if you can get the vaccine on the NHS.
Page last reviewed: 23 November 2023
Next review due: 23 November 2026