Psoriatic arthritis is a long-term condition that causes joint pain, swelling and stiffness. Medicines can help treat the symptoms.
Some people with the skin condition psoriasis will get psoriatic arthritis as they get older.
Check if you have psoriatic arthritis
Symptoms of psoriatic arthritis include:
- pain, swelling and stiffness in 1 or more joints
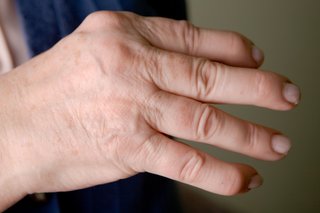
- swollen fingers or toes
- your nails changing from their usual colour, or tiny dents or pits developing in your nails
- feeling drained of energy
Symptoms can be worse first thing in the morning and may improve with exercise.
Some people may also get symptoms of psoriasis, such as dry scaly skin, at the same time.
If you're not sure it's psoriatic arthritis
There are other conditions that can cause joint pain, stiffness and swelling, including:
Non-urgent advice: See a GP if:
- you have joint pain, stiffness and swelling that keeps coming back
You should see a GP even if you do not have psoriasis. These symptoms need to be checked.
What happens at your appointment
If the GP thinks you may have psoriatic arthritis, they'll refer you to a specialist (rheumatologist).
Tests you may have include:
- blood tests
- joint fluid test – where fluid is removed from an affected joint and tested
- X-rays, ultrasound scans and MRI scans
Treatments for psoriatic arthritis
Medicines are the main treatment for psoriatic arthritis. If a medicine does not help with your symptoms tell your doctor. Another medicine may work better for you.
Medicines for psoriatic arthritis
The medicines used to treat psoriatic arthritis include:
- non-steroidal anti-inflammatory drugs (NSAIDs) – they come as tablets, creams or gels and can help with mild symptoms
- steroid injections – a steroid medicine is injected into a joint to help ease the pain
- disease-modifying anti-rheumatic drugs (DMARDs) – used for moderate to severe symptoms, DMARDs can take several months to work so keep taking them even if you do not feel better straight away
- biological treatments – usually given by injection, biological treatments can be used if DMARDs do not help
Other treatments for psoriatic arthritis
Your doctor may also refer you to a physiotherapist, occupational therapist, or both.
A physiotherapist can teach you exercises to help strengthen your joints and prevent joint damage.
An occupational therapist can discuss adjustments you can make at home and at work. For example, they may recommend equipment that makes certain tasks easier.
More information
Things you can do to ease the symptoms of psoriatic arthritis
There are some things you can do to help ease the symptoms of psoriatic arthritis.
Do
-
exercise regularly – low impact exercises like swimming, walking and yoga can help strengthen and protect your joints
-
try to lose weight if you're overweight to reduce pressure on your joints
-
cut down on alcohol if you're taking medicines – alcohol can affect medicines
Don’t
-
do not smoke because it can make symptoms of psoriatic arthritis worse
-
do not use herbal remedies because they may interfere with any medicines you're taking
Causes of psoriatic arthritis
Some people with psoriasis get psoriatic arthritis.
It can sometimes develop after you've had psoriasis for many years.
Like psoriasis, psoriatic arthritis is caused by the immune system attacking healthy tissue.
It's not clear why some people with psoriasis get psoriatic arthritis but others do not.
Page last reviewed: 06 September 2023
Next review due: 06 September 2026