Hives rashes usually get better within a few minutes to a few days. You can often treat hives yourself.
Check if it's hives
The main symptom of hives is an itchy rash.
The rash can:
- be raised bumps or patches in many shapes and sizes
- appear anywhere on the body
- be on 1 area or spread across the body
- feel itchy, sting or burn
- look pink or red when affecting someone with white skin; the colour of the rash can be harder to see on brown and black skin
- 1: White skin with hives rash (thumbnail).
- 2: White skin with hives rash (thumbnail).
- 3: Hives rash on light brown skin (thumbnail).
- 4: Hives rash on light brown skin (thumbnail).
- 5: Hives rash on light brown skin (thumbnail).
- 6: Dark brown skin with hives rash (thumbnail).
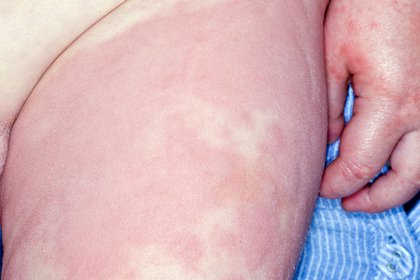
Long description, image 1.
Hives rash on the leg and hand of a child with white skin.
The skin on most of their thigh is pink, raised and bumpy. At the side of their thigh, close to their hand, are deep creases in the skin.
Their hand is pink with some red patches between their thumb and finger and on their fingertips.
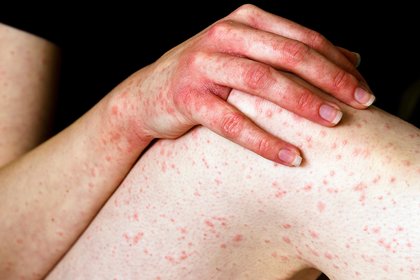
Long description, image 2.
Hives rash on the leg, arm and hand of a person with white skin.
Small, slightly raised pink spots cover their leg. Some are close together and some are further apart.
The same spotty rash spreads along the side of their arm and across the top of their hand. The knuckles and fingertips are red.
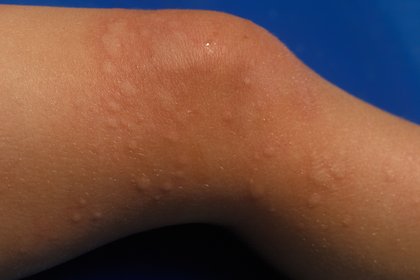
Long description, image 3.
Hives rash on the knee of a person with light brown skin. The skin is slightly darker brown around where the rash is.
There are many skin-coloured bumps on and around the knee which vary in size from around 2mm to 1cm. The larger bumps look puffy like blisters. Some bumps are very close together in groups.
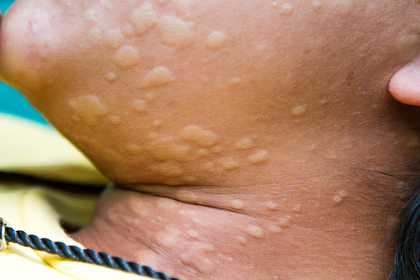
Long description, image 4.
Hives rash on the cheek, chin and neck of a person with light brown skin.
There are about 50 raised bumps in different shapes and sizes.
Some of the bumps are small circles and others are larger, uneven shapes. Most are close together in groups, but some are further apart. The bumps are a lighter brown than the surrounding skin and look puffy, like blisters.
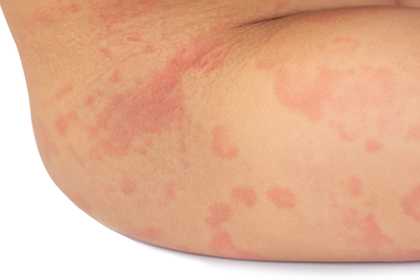
Long description, image 5.
Hives rash on the thigh and hip of a child with light brown skin.
There are about 20 patches of pink skin in different shapes and sizes. The patches are mainly flat and vary in size from around 1cm to 8cm.
Some patches are close to or join others, while some are further apart.
Some patches are dark pink. Others are lighter pink with a darker pink border around the patch.
There's a long, dark pink patch spreading from their groin to their hip.
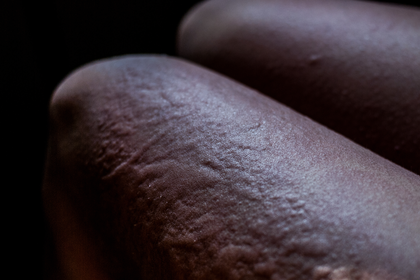
Long description, image 6.
Hives rash on the thigh of a person with dark brown skin.
There are many raised patches of skin in different shapes and sizes very close to each other. They range from around 5mm to 5cm.
The skin near the left knee also has raised lines, like scars. The skin on the inside of the thigh is smooth.
The rash is the same colour as the person's skin.
If you're not sure it's hives
Look at other rashes in babies and children.
A pharmacist can help with hives
A pharmacist can give you advice about antihistamine treatment to help a hives rash.
Tell the pharmacist if you have a long-term condition, because you might not be able to take antihistamines.
This treatment might not be suitable for young children.
Non-urgent advice: See a GP if:
- the symptoms do not improve after 2 days
- you're worried about your child's hives
- the rash is spreading
- hives keeps coming back (you may be allergic to something)
- you also have a high temperature and feel unwell
- you also have swelling under your skin (this might be angioedema)
Immediate action required: Call 999 if:
- your lips, mouth, throat or tongue suddenly become swollen
- you're breathing very fast or struggling to breathe (you may become very wheezy or feel like you're choking or gasping for air)
- your throat feels tight or you're struggling to swallow
- your skin, tongue or lips turn blue, grey or pale (if you have black or brown skin, this may be easier to see on the palms of your hands or soles of your feet)
- you suddenly become very confused, drowsy or dizzy
- someone faints and cannot be woken up
- a child is limp, floppy or not responding like they normally do (their head may fall to the side, backwards or forwards, or they may find it difficult to lift their head or focus on your face)
You or the person who's unwell may also have a rash that's swollen, raised or itchy.
These can be signs of a serious allergic reaction and may need immediate treatment in hospital.
Treatment for hives from a GP
A GP might prescribe menthol cream, antihistamines or steroid tablets.
If hives does not go away with treatment, you may be referred to a skin specialist (dermatologist).
You cannot always prevent hives
You get hives when something causes high levels of histamine and other chemicals to be released in your skin. This is known as a trigger.
Triggers can include:
- eating certain foods
- contact with certain plants, animals, chemicals and latex
- cold, such as cold water or wind
- hot, sweaty skin from exercise, emotional stress or eating spicy food
- a reaction to a medicine, insect bite or sting
- scratching or pressing on your skin, such as wearing itchy or tight clothing
- an infection
- a problem with your immune system
- water or sunlight, but this is rare
Try to find out what triggers hives for you, so you can avoid those triggers, if possible. This may help prevent an episode of hives.
Page last reviewed: 13 April 2021
Next review due: 13 April 2024