Lichen planus is a rash that can affect different parts of your body, including the inside of your mouth. See a GP if you think you might have it.
Check if it's lichen planus
The main symptoms of lichen planus include:
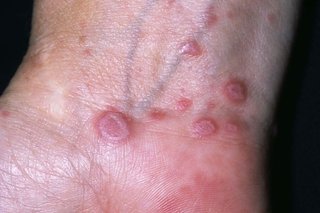
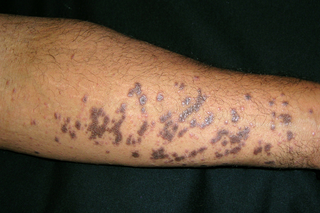
- clusters of shiny, raised, purple-red blotches on your arms, legs or body (you may see fine white lines on the blotches) – the rash may be harder to see on black or brown skin
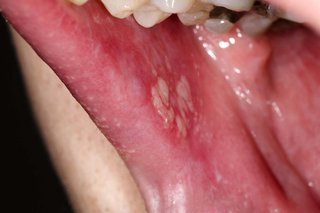
- white patches on your gums, tongue or the insides of your cheeks
- burning and stinging in your mouth, especially when you eat or drink
- bald patches appearing on your scalp
- sore red patches on your vulva
- rough, thinning nails with grooves on
- ring-shaped purple or white patches on your penis
You may only have 1 of these symptoms.
Lichen planus on your skin can be very itchy, but not always.
If you're not sure it's lichen planus
| Symptoms | Possible cause |
|---|---|
|
Red, flaky, crusty patches, often on elbows or knees |
|
|
Raised, red, scaly patches on the body |
|
|
Itching and white patches on the vulva |
|
|
Ring-like red patch anywhere on the body |
|
|
Itchy, dry, cracked, sore and red skin |
Eczema |
Non-urgent advice: See a GP if:
- you think you have lichen planus
Treatments for lichen planus
Lichen planus on your skin usually gets better on its own in about 9 to 18 months.
Creams and ointments from a GP can help control the rash and ease itching.
If creams and ointments do not work, or you have severe lichen planus, steroid tablets or treatment with a special kind of light (light therapy) can help.
Lichen planus in your mouth can last for several years. Mouthwashes and sprays from a GP can help ease symptoms like burning or sore gums.
You cannot catch lichen planus and it does not usually come back once it's cleared up.
How to ease lichen planus at home
There are things you can do to help ease lichen planus symptoms at home. These will depend on which area of your body is affected.
Lichen planus on the skin
If you have lichen planus on your skin:
- wash with warm water – avoid soaps and body washes
- wash your hair over a sink or bath so the shampoo does not touch the rest of your skin
- a GP may prescribe a moisturising treatment for the skin (emollient) to use on the rash
- try not to scratch your skin
Lichen planus on the genitals
If you have lichen planus on your genitals:
- try to have showers rather than baths
- hold a bag of frozen peas wrapped in a clean tea towel against the affected areas to ease itching and swelling
- avoid wearing tights or close-fitting clothes
- carefully dry yourself after having a pee to reduce the chances of pee getting in contact with your skin – avoid rubbing the area
- use a lubricant if sex is painful
Lichen planus in the mouth
If you have lichen planus in your mouth:
- avoid salty, spicy and acidic foods, or alcohol, if they make your mouth sore
- brush your teeth carefully twice a day to keep your gums healthy
- use a mouthwash that does not contain alcohol, if it makes your mouth sore
Page last reviewed: 02 August 2023
Next review due: 02 August 2026